What is the carpal tunnel?
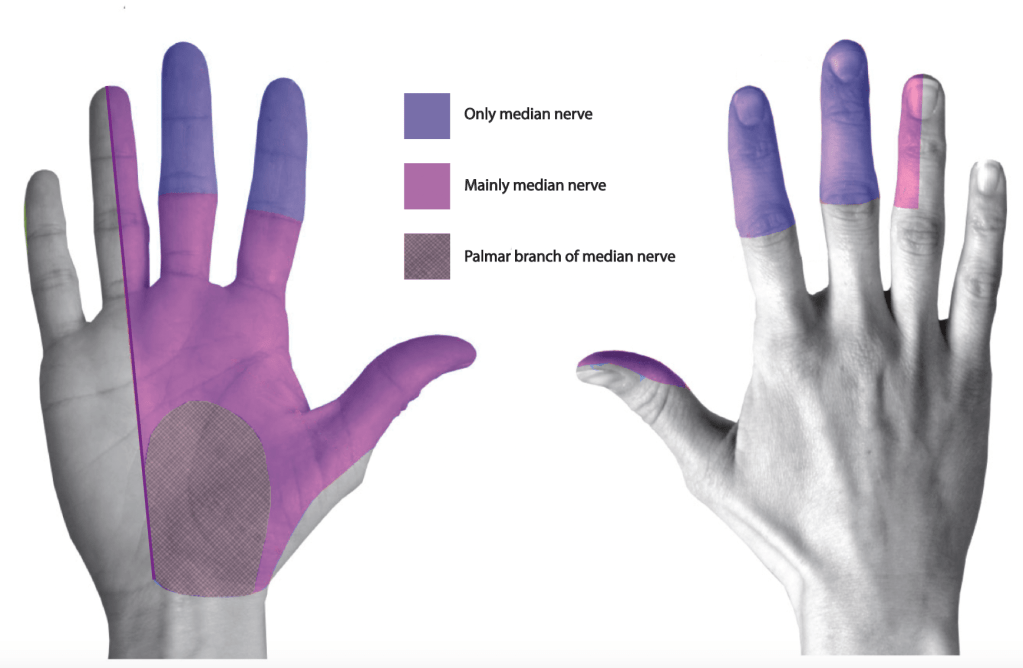
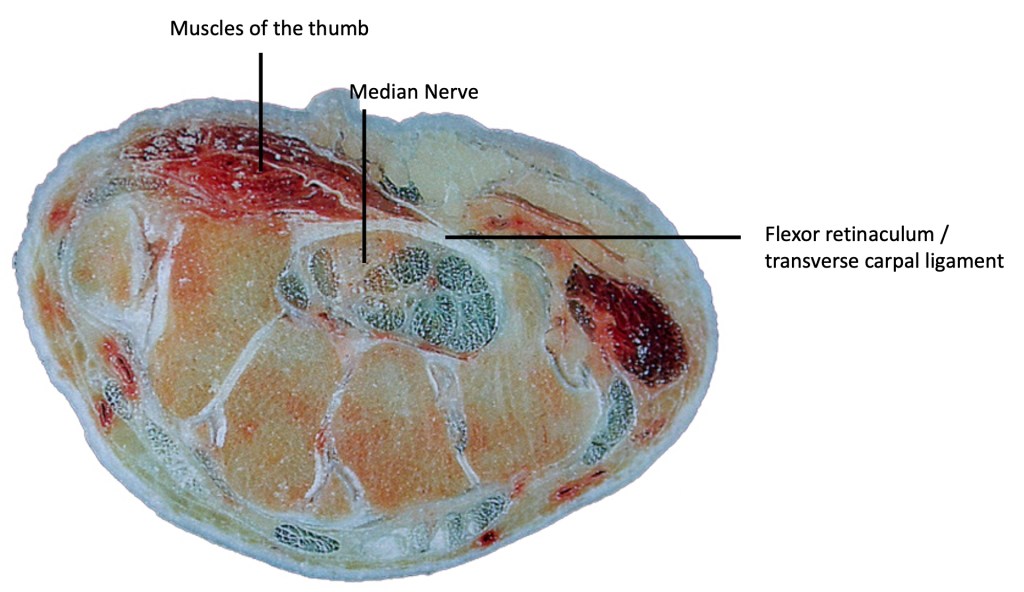
At the base of the hand, there is a ligament called the transverse carpal ligament or also known as the flexor retinaculum (see diagram below). A large nerve (the median nerve) and all the tendons that bend the fingers and thumb pass underneath this ligament on their way from the forearm into the hand. The space below the ligament is known as the carpal tunnel. The median nerve supplies sensation to the fingers, and some of the hand muscles (diagram below).

What is carpal tunnel syndrome?
Carpal tunnel syndrome (CTS) is a condition where the median nerve is compressed as it passes through the carpal tunnel. When it is compressed, the nerve starts to malfunction, producing symptoms.
What are the symptoms of carpal tunnel syndrome?
– Tingling and numbness in the hand This affects the part of the hand supplied by the median nerve (see picture below), and often feels like the whole hand is tingling.
– Night time symptoms Symptoms tend to wake people from sleep, and many people find that hanging their hand out of the bed or shaking it will relieve the symptoms.
– Difficulty with fiddly tasks As the condition gets worse, the numbness and tingling can become constant with altered sensation in the hand and inability to feel things properly.
– Weakness of pinch grip When the condition becomes severe, then the muscles of the thumb can become weak.
Click here to find out if your symptoms might be due to carpal tunnel syndrome
Who gets carpal tunnel syndrome?
Most people who get carpal tunnel syndrome have no obvious cause for developing the condition, and the tendency to get it is largely from genetic factors.
As people age, the space in the carpal tunnel becomes less. This can be enough to produce symptoms from the condition. Although carpal tunnel syndrome can present at any age, but it is rare in children and young adults, becoming more common in middle age.
Other things, such as diabetes, underactive thyroid, arthritis and trauma can affect when people develop symptoms.
How is it diagnosed?
In many cases the diagnosis can usually be made based on patient symptoms and examination. There are two tests used by surgeons to help make the diagnosis: Phalen’s test is a simple manoeuvre where the wrist is allowed to flop down with gravity when the elbow in on a table. This manoeuvre increased the pressure within the carpal tunnel and in patients with carpal tunnel syndrome, this will give rise to tingling in the area supplied by the median nerve.

Tinel’s sign involves lightly tapping over the nerve to detect an area of irritation. This will produce a tingling sensation in the hand if the test is positive.
A test to measure nerve impulses (nerve conduction study) will usually confirm the diagnosis, and give an idea as to how severe the problem is. This study involves a doctor or specialist technician placing some sticky pads on the arm and measuring the speed taken for signals to be transmitted down the nerve. It can feel uncomfortable but is not usually painful.
What is the natural history?
In many patients, symptoms from carpal tunnel syndrome can come and go for some time before becoming a problem. Treating any contributing problem such as diabetes or thyroid disease may improve symptoms. Carpal tunnel syndrome in pregnancy often will get better after the baby is born, but may return some years later.
If the condition continues to worsen, then it is important to talk to your doctor about the symptoms. The condition is easy to treat when the symptoms are bothersome but still coming and going. Although nerve function can get worse with time, it is easy to make sure this doesn’t happen by treating it before it gets to this stage.
What is the treatment?
1) Splinting – A wrist splint with the wrist in a straight or neutral position can help improve symptoms if worn at night, but not always. Buy a wrist splint here.
2) Steroid Injection – A steroid injection into the carpal tunnel can help improve symptoms in the short term, usually around three months. It has no proven lasting benefit. Steroid injection is often recommended if there are reasons why surgery to the hand would be inconvenient for work or for other reasons. Having a steroid injection
3) Surgery – Surgery remains the most effective, proven long-term solution to Carpal Tunnel Syndrome. The operation involves cutting the ligament over the front of the wrist to ease the pressure on the nerve. The surgery is routinely done under local anaesthesia.

This usually cures the problem. Night pain and tingling usually disappear within a few days. In severe cases, constant numbness and muscle weakness may be slow to get better or may not be much better than before surgery. Occasionally pain can be felt over the inside of the wrist. It generally takes many months to get back full strength and a comfortable scar. The hand can be used for light activities from the day of surgery.
Although surgery is a relatively safe option with excellent one year outcomes, there is a price to pay. Since the surgeon divides the ligament at the front of the wrist (flexor retinaculum / transverse carpal ligament), the normal function of this ligament is lost for a while, before the ligament reforms with scar tissue.
- There can be a feeling of instability for the first few months when using the hand for anything heavy, or a dull ache across the base of the hand when pushing up from a chair or bath. In patients with pre-existing arthritis of the wrist, arthritic symptoms can be exacerbated by loss of the ligament. These symptoms improve with time and are generally not an issue at the one year follow up.
- The flexor tendons (tendons responsible for grip) lose one of the ‘pulleys’ used to increase their efficiency. Loss of the ligament usually results in loss of grip strength, although this recovers over the course of around one year, and is usually normal in the long term.
- The small muscles of the hand that work the thumb and little finger normally pull from the ligament. When the ligament is divided, it makes pinch grip difficult for the first few weeks. Again, this tends to improve with time and returns to normal within a year.
Overall, the results of open carpal tunnel decompression are excellent with around 96% of patients reporting good outcomes at one year. There are risks involved with all surgery, however, and you can read more about these risks here.

© Fife Hand Service 2023