What is osteoarthritis?
The term ‘arthritis’ is used to describe a swelling in a joint. There are many different types of arthritis, and osteoarthritis is the most common. It is also known as ‘wear and tear’ arthritis, although this is not a good name, as the condition in the hands is rarely a result of how the hands are used, and far more commonly a result of the normal ageing process and genetics. Osteoarthritis can also occur as a result of injury to a joint, and this is known as ‘secondary osteoarthritis’.
The term osteoarthritis, therefore, is used to describe the process of swelling of the hand joints, with associated bony spurs, loss of normal joint cartilage (the smooth surface of the joint) and consequent pain and stiffness.

Why does it occur?
Osteoarthritis in the hands develops primarily as a result of genetic tendency and normal ageing. On an X-ray, there is always a gap between the bones. Because the smooth cartilage overlying the bone does not show up on an X-ray, the amount of cartilage left in a joint can be measured as the distance between the bones on an X-ray. This gap is big in children and young adults, and narrows as people age, so that by around 50 years, it is significantly less than at 30, and by 80, it is usually pretty small.
As the joint surface or cartilage wears, the normal ligaments which hold the joint firm and stable become loose, allowing the joints to become a little unstable. The bone reacts by making more bone around the edges of the joint to try and keep the joint as stable as possible. Within the joint, inflammation can develop, making the process painful.
What is the natural history?
The natural history is a term used to describe what happens when nature runs its own course. With osteoarthritis in the hand, it is often possible to see what is likely to happen with time by looking at the hands of parents, since this is often hereditary. Most people will find that although their parents may have quite stiff and misshapen hands, their hands still work fairly normally and there is not much that they are unable to do because of the arthritis.
The majority of people develop changes of osteoarthritis with time, but for most, the condition is not terribly painful, although individual joints can flare up from time to time. In some patients, however, the joint becomes inflamed and this produces pain. The inflamed painful joint will often last anything from a few months to a few years, but usually ‘burns out’ with time. This ‘burn out’ means that the inflammation and pain eventually settle, although the joint is often quite stiff and sometimes deformed by this stage.
People who have a strong family history of osteoarthritis tend to report that single joints flare intermittently, and the process moves on to another joint when the arthritis burns out of one.
Rarely, an individual can have a severe form of osteoarthritis, usually if this runs in the family. This can mean that some or all of the joints flare at once, and the accompanying pain and inflammation can be severe.
Generally speaking, as the condition progresses, the hands tend to become stiffer, such that the hand does not easily close into a fist, and may not straighten fully.
Making the diagnosis
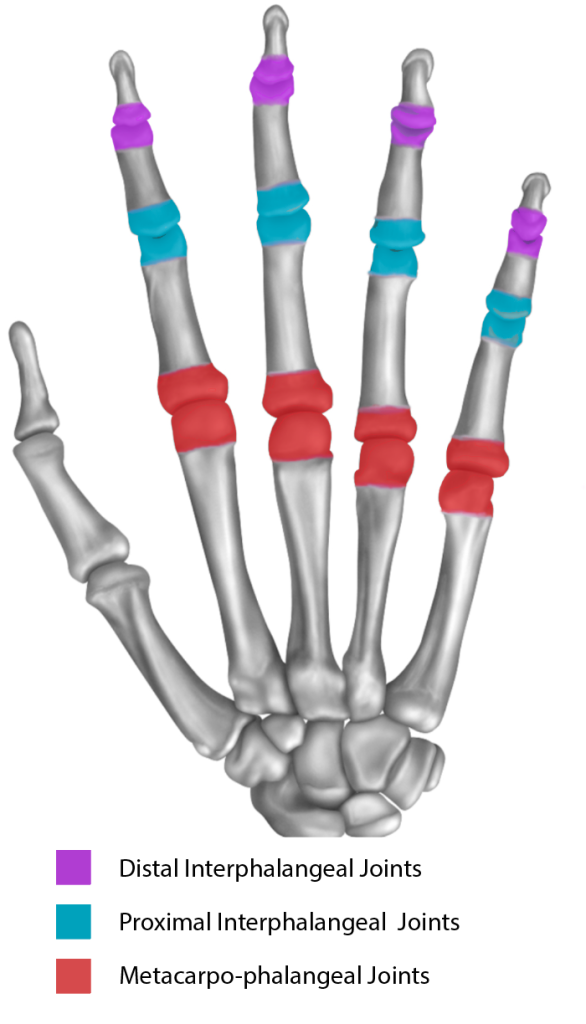
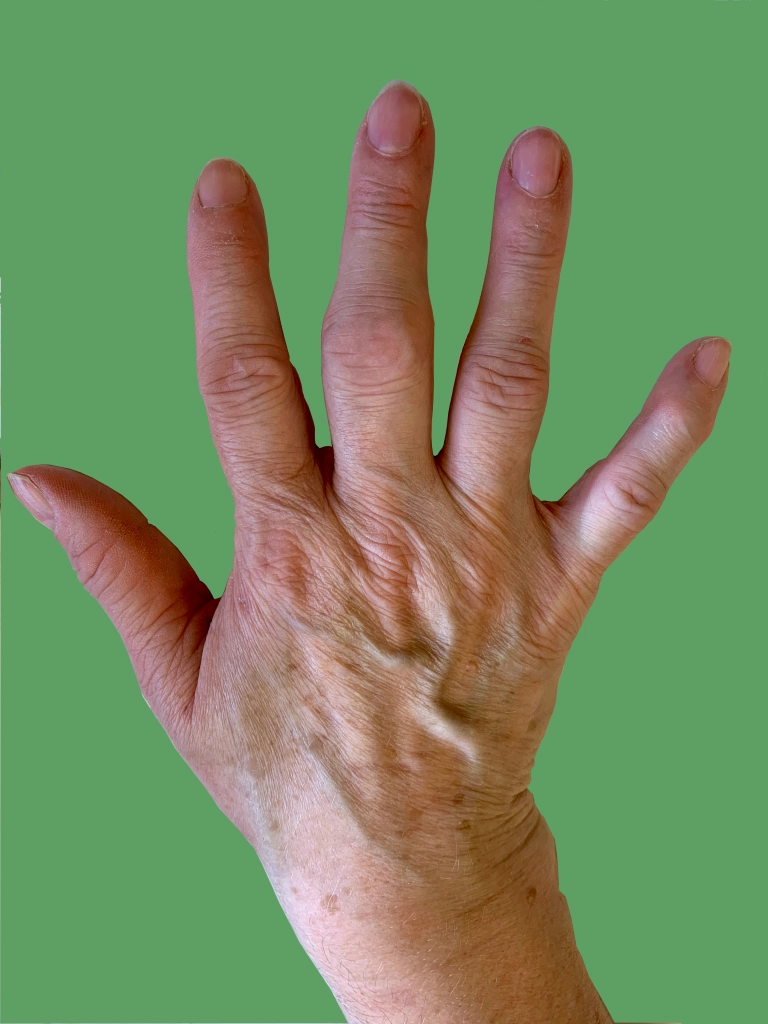
The diagnosis is made on clinical examination of the hands. Heberden’s nodes are bony lumps arising from the distal interphalangeal joints. Bouchard’s nodes arise from the proximal interphalangeal joints. The metacarpo-phalangeal joints are often spared. An X-ray will usually confirm the diagnosis. If there is a possibility of the arthritis being a type other than osteoarthritis, then a blood test may be recommended.
You can read about how osteoarthritis is diagnosed on an X-ray here.
Treatment:
Non-operative treatment
Pain is the body’s defence mechanism to alert the brain to the possibility of harm. Pain is usually a protective mechanism and helps people avoid burns and cuts, or alerts to something which has ‘gone wrong‘ in the body. Pain from osteoarthritis can, therefore, make people worry about their hands – and this worry usually has two forms:
1) If my hands are painful now, what will they be like in a year or two?
Although slow deterioration is usual with osteoarthritis, generally speaking pain burns out with time, and the chances of symptoms being much worse in a year or two are slim.
2) If it is painful to use my hands, am I doing any harm by using them, and should I rest them? Actually, there is no harm in using arthritic hands normally. Normal use of the hand does not cause the condition to worsen – ageing and genetics are responsible for the rate of deterioration.
So it is quite safe to use the hands normally and to do usual activity despite the pain. With this reassurance, many people do not require any treatment for their arthritis. If the pain is preventing normal use, then the following steps can be useful:
- Splints – sometimes immobilising a joint will allow the hand to work comfortably
- Physiotherapy – working to maintain movement can delay the onset of stiffness
- Simple painkillers – Although painkillers can be useful from time to time, the routine use of painkillers is not recommended. All painkillers carry a risk from the side effects, and although some painkillers such as ibuprofen can be effective for this type of pain, regular use can give rise to complications such as a stomach ulcer or cardiac problems. Stronger painkillers can be addictive and are not recommended.
- Steroid Injection – Steroid injections can provide pain relief for a single troublesome joint, by reducing the inflammation in the joint. Steroid injections are not given into the fingertip joints, but are offered in the other finger joints if appropriate. These injections carry a risk and do not usually provide anything other than short term pain relief. See our information on Having a steroid injection
What operations can help?
There are two types of operation which can produce pain relief in an arthritic joint:
Joint replacement surgery – Some of the knuckle joints can be replaced with a plastic hinge joint, which will remove pain from the arthritis but will also completely alter the way the hand works. Joint replacements tend to wear out within a few years in the hand, and are often associated with loss of grip strength. Other metal or carbon joint replacements are also available for the finger joints, but we do not offer these routinely in Fife, because there is no good evidence to back up the use of these implants over the natural history of the condition. Complications from joint replacements include infection, loosening or breakage of the joint, and dislocation, but also the other risks outlined in our information sheet on Having a hand operation.
Joint fusion surgery – Fusion is the term used when the joint in removed and the bones on either side of the joint are pinned together so that they heal over with bone. This type of surgery sacrifices movement for pain relief, but can be useful particularly for the fingertip joints. Complications include infection, failure of the bone to fuse, and irritation from the pins holding the bones in place, as well as the other risks outlined in our information sheet on Having a hand operation.

© Fife Hand Service 2023