Diabetes increases the incidence of many common hand conditions. This page outlines the effects of diabetes on the hand, and the outcomes following surgery for these conditions.
Why does diabetes affect the hand?
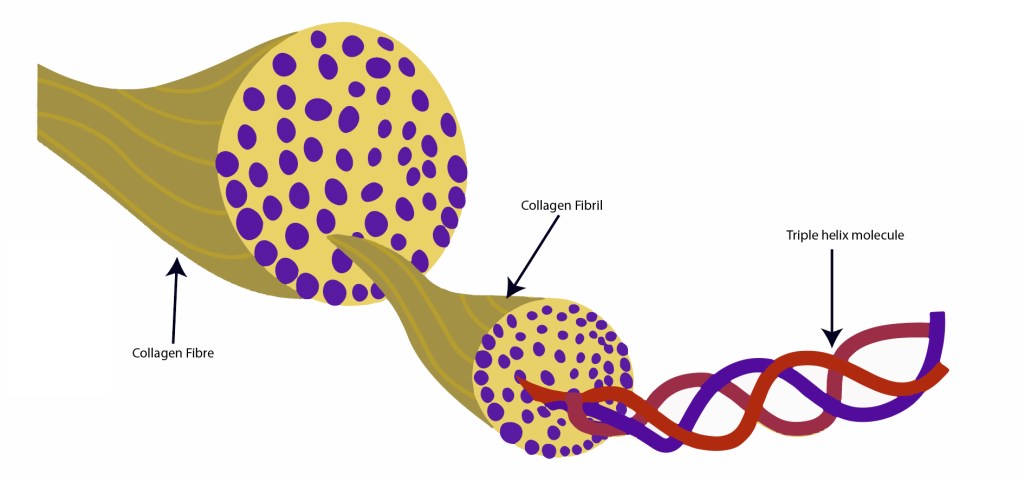
All soft tissues in the body contain collagen. Collagen is a molecule made up of three strands of protein which are bundled into fibres. Collagen is the ‘binding’ protein – or the protein responsible for binding the body together.
In diabetes, excess sugar in the cells bonds with the collagen molecules, and produces links between the collagen molecules that should not be there. The basic structure of the collagen is very slightly altered. The collagen becomes stiffer in comparison to how it would be without these cross links and then behaves differently as a result.
Carpal Tunnel Syndrome
Carpal tunnel syndrome is a condition where the median nerve is compressed as it runs though the carpal tunnel at the wrist. It is very common and surgery to release the carpal tunnel is one of the most common operations performed in the NHS. You can read more about Carpal Tunnel Syndrome here.
How does diabetes affect carpal tunnel syndrome?
Hand function in patients with diabetes presenting with carpal tunnel syndrome is usually not quite as good as in patients without diabetes. At 1 year following surgery to decompress the carpal tunnel, hand function has improved significantly in both patients with diabetes and those patients without; with similar improvement in both groups. The starting point, however, is worse and therefore the end point is similarly worse compared to patients without diabetes. Satisfaction rates are similar in both groups, with 96% of patients reporting good or excellent outcomes at 1 year.
Trigger Finger
Trigger finger is a mechanical problem affecting the tendons as they run into the finger. This can cause a click, and sometimes finger can become stuck in a bent position. You can read about Trigger Finger here.
How does diabetes affect trigger finger?
Patients with trigger finger who have diabetes are more likely to have multiple trigger digits than those without diabetes. In addition, resolution of the trigger following a single steroid injection is less likely in patients with diabetes.
Functional improvement following surgery for a trigger finger is the same in patients with diabetes compared to patients without diabetes, although the starting function and final function scores are generally poorer in those patients with diabetes.
Dupuytren’s Disease
Dupuytren’s disease is a condition in which scar tissue forms in the specialised fascia of the hand, and which eventually produces contracture of the fingers. You can read more about Dupuytren’s Disease here.
How does diabetes affect Dupuytren’s Disease?
Since Dupuytren’s disease has a strong genetic component, patients with diabetes but without the genetic predisposition remain unlikely to get this condition. However, the genetics are complex and not yet fully understood.
Surgery for this condition is tricky and involves dissection of nerves and tiny blood vessels in the fingers. Any pre-exisiting vascular disease is likely therefore to be aggravated by this type of surgery, and surgeons tend to recommend against dermofasciectomy in patients who have poor control of their diabetes because of this.
The outcome of surgery for Dupuytren’s disease is notoriously difficult to measure, but the satisfaction rates following surgery are the same in both patients with diabetes and those without.
Diabetic Neuropathy
Diabetic neuropathy is a complication of diabetes caused by damage to the nerve cells, particularly the smaller nerves. This can cause pain, but more commonly numbness in the hands. The symptoms of neuropathy are similar to the symptoms from carpal tunnel syndrome, but clinical examination will usually distinguish between reversible compression and irreversible nerve damage. This can be confirmed with a nerve conduction study.
The mechanism by which the nerve cells are damages is complex and multifactorial. Higher levels of tissue sugar alters the ‘soup’ in which the nerve cells are bathed, and causes damage to the specialist myelin sheath cells, which insulate the nerve and allow the electrical signals to pass down the nerve smoothly.
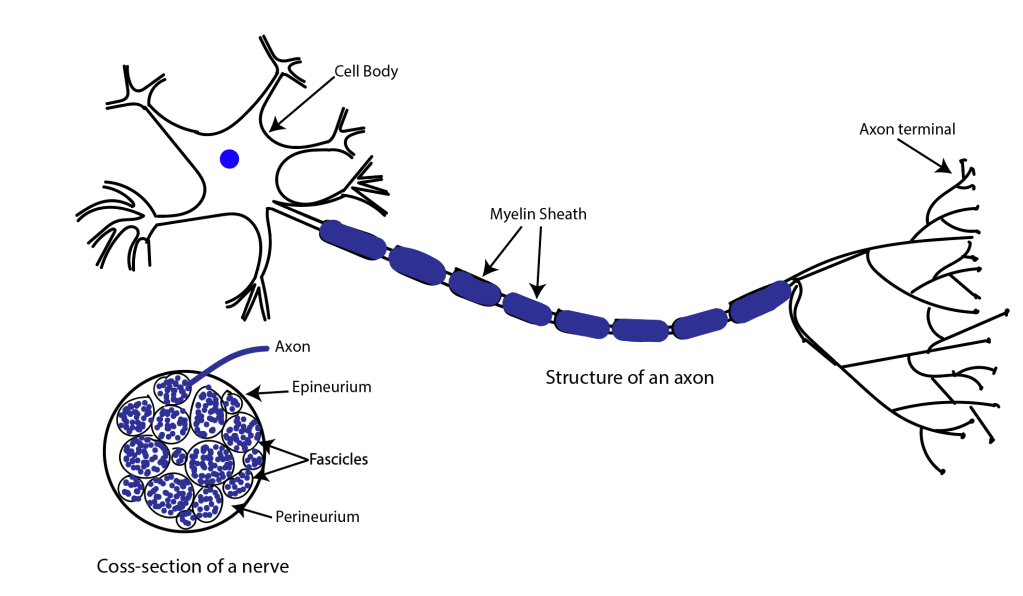
As this sheath is damaged, the nerve becomes ‘demyelinated’ and stops working effectively. The smaller nerves are affected first in diabetes, and this means that nerves in the fingertips (and toes) are usually the first to give problems.
Whereas a nerve compression such as carpal tunnel syndrome gives rise to symptoms in the distribution of a particular nerve, diabetic peripheral neuropathy classically what is known as a ‘glove and stocking‘ distribution.
Diabetic neuropathy does not respond to surgery, and the best management is tight sugar control in order to avoid any deterioration once the diagnosis is made.
Raynaud’s Disease
This is a manifestation of the ‘microvascular’ disease seen in patients with diabetes. It affects the very smallest blood vessels, particularly in the fingertips (and toes). It is characterised by the fingers becoming white intermittently, with poor capillary return – this is a measure of the time it takes for the fingertip to become pink after it is blanched with pressure.
The presence of this condition can adversely affect the recovery from surgery in the hand, particularly Dupuytren’s surgery. It is also markedly exacerbated by smoking, which is an independent common cause of this disease too, so smoking and diabetes are not a good combination. Actually, smoking has no proven benefits – just risks!
Diabetic Cheiroarthropathy
Diabetic cheiroarthropathy translates roughly as ‘stiff joints‘, and this is exactly what happens! It is again related to structural changes in the collagen of the soft tissues, and is more common in longstanding diabetes. In its early stages, many patients do not notice the loss of full extension and inability to bring the hands together in a prayer posture (see below). As is develops, the flexion contractures of the small joints prevent the hands from opening fully, and eventually the process also affects the ability to bring the hands into a fist.
It is difficult to alter the natural history of this complication of diabetes. Tight sugar control may slow the process, and hand therapy is often useful to maintain movement and try to regain lost movement. There is no place for surgical management with this condition.


© Fife Hand Service 2023